In 2019, almost 50,000 people in the US died as a result of opioid overdose; this number includes events involving prescription pain medications, heroin, and synthetic opioids like fentanyl. The CDC estimates the annual economic burden of prescription opioid misuse at $ 78.5 billion.¹
It’s important for everyone to learn about naloxone (also known by the name brand Narcan), its uses, and limitations — give yourself the ability to save someone’s life. UW-Madison is a participant in Wisconsin Voices for Recovery’s Nalox-ZONE Program and provides free access to naloxone in 25 locations on campus. All UWPD officers also carry naloxone with them.
You don’t need a full class to help someone with naloxone. If you want to learn more and better prepare to help someone in an emergency UWPD and RecWell offer First Aid/CPR/AED classes regularly.
What is naloxone and how does it work?
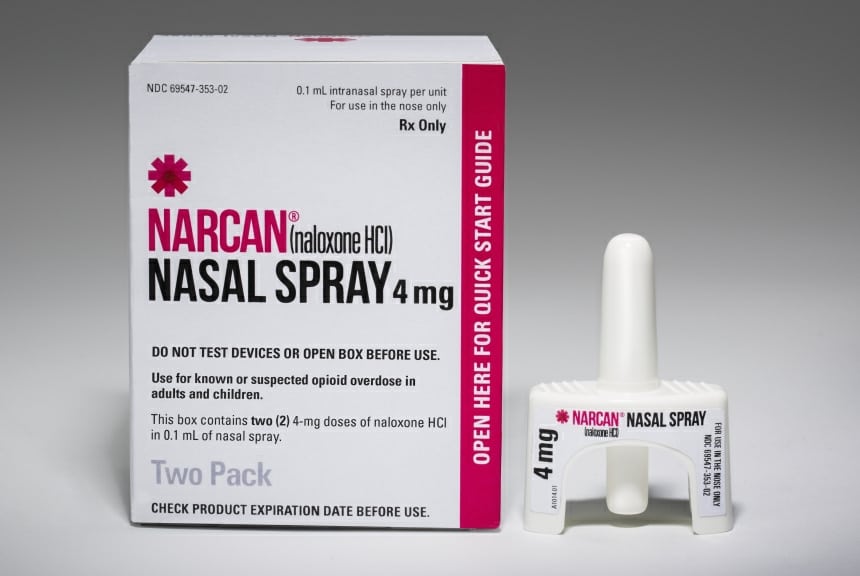 Naloxone is an opioid antagonist. Instead of counterbalancing symptoms like Epinephrine (EpiPen) to overcome the effects of an extreme allergic reaction, naloxone blocks the brain’s uptake of opioids by replacing them. Think of your brain cells like a toddler’s shape sorter toy — the one with the different shaped holes and blocks. Naloxone comes along and replaces the opioid. It can boot it out or fill the hole before the heroin comes along.
Naloxone is an opioid antagonist. Instead of counterbalancing symptoms like Epinephrine (EpiPen) to overcome the effects of an extreme allergic reaction, naloxone blocks the brain’s uptake of opioids by replacing them. Think of your brain cells like a toddler’s shape sorter toy — the one with the different shaped holes and blocks. Naloxone comes along and replaces the opioid. It can boot it out or fill the hole before the heroin comes along.
Naloxone does not treat overdoses of non-opioid medications, and it does not have an effect on someone who has not taken opioids.²
Risk Factors for Opioid Overdose
Although any opioid use can lead to overdose, some factors that may increase overdose risk include:
- combining opioids with alcohol or other drugs (such as benzodiazepines)
- taking a high daily dosage of opioids
- taking more opioids than prescribed by the physician
- taking illegal opioids that could contain unknown substances
- having sleep apnea, impaired hepatic or renal function
Signs of an opioid overdose include:
- slowed or shallow breathing (or no breathing)
- pinpoint pupils (small, constricted pupils)
- falling asleep
- loss of consciousness
- choking or gurgling
- limp body
- skin that is pale, blue, and/or cold
In the event of an opioid overdose (or suspected overdose), administer naloxone and call 911. Keep the person awake and talking. Another naloxone dose (or more) may be necessary. Stay with the person until emergency help arrives.
Adverse Effects
Naloxone may cause withdrawal symptoms. Although uncomfortable, withdrawal symptoms are not life-threatening. They may include headache, blood pressure changes, tachycardia, sweating, nausea, vomiting, tremors, irritability, nervousness, aggressive behavior, body aches, fever, runny nose, and sneezing.
But I don’t want my friend to get into trouble. Do I have to call 911?
YES — you do. Naloxone is fast acting and temporary — whereas opioids can be very long lasting. The overdose victim can often succumb to the opioids again as soon as the naloxone wears off. They can slip back into unconsciousness and stop breathing all over again! That’s why it’s so important to call 911 if you administered naloxone to anyone. The threat of relapse into life-threatening symptoms is very real and occurs regularly. The victim must be helped through the overdose by medical professionals.
Keep in mind: UW’s Medical Amnesty Through Responsible Actions program extends from alcohol to opioids — and many other things in between. If you call because you are concerned for someone’s health, and you cooperate with first responders, please know UWPD will not take enforcement action on anyone who calls and stays to help in an emergency.
¹ Opioid overdose crisis. National Institute on Drug Abuse. Updated March 11, 2021. Accessed May 23, 2021. https://www.drugabuse.gov/drug-topics/opioids/opioid-overdose-crisis
² Naloxone. National Institute on Drug Abuse. Updated September 2019. Accessed May 23, 2021. https://www.drugabuse.gov/publications/drugfacts/naloxone
